OpenGov Voices: Will a recent court decision jeopardize open data in health care?

At first glance, the recent Supreme Court decision in Gobeille v. Liberty Mutual signals an end for state efforts to collect and disseminate de-identified health claims data with the intent of creating more efficient and competitive health care markets. Years of hard work, collaboration and progress on behalf of state policymakers and the private sector now feels like a bona fide Sisyphean effort.
Without getting into details of the legal basis on the Gobeille case, the initial “read” of the decision is that consumers will just have to muddle through the black abyss that is today’s byzantine health care maze. The ruling is a blow for open data advocates pushing for more transparency and accountability.
The Supreme Court’s message from the ruling is clear: Move along, nothing to see here. Evidently, we don’t need to know how much we are paying for our health care as we face the highest cost sharing schemes in history. But we want and deserve answers.
Who is doing the dirty work?
Liberty Mutual, a self-funded company, contracts to Blue Cross Blue Shield of Massachusetts (BCBS) to administer the health claims for its 80,000 employees. Fewer than 100 of those employees work in Vermont – one of at least 18 states working on or that have already implemented state-based, all-payer claims databases. In reality, BCBS already submits claims to various state all-payer claims databases on behalf of thousands of companies and hundreds of thousands of individuals. The company was not even required to quantify the financial burden because its argument was based on a technical legal interpretation of ERISA pre-empting state laws.
It’s time to call it what it is
The dirty secret here that is Liberty Mutual argued the case all the way to the Supreme Court for seemingly no good, self-serving financial reason other than to help BCBS. Take a look at Liberty Mutual’s board lineup: Notice any directors that have ties to BCBS of Massachusetts? Think there is any back scratching that goes on at those Fenway luxury boxes? What’s even more puzzling is why no one seems to care about this. Are we just too beaten down from the flawed political process and special interest groups that heavily influence both parties in Washington? The fact is some government still works reasonably well, at least at the state level. Consumers need to defend our respective state’s rights and insist that ERISA shortfalls are addressed. What’s the alternative? Do we wait until health care becomes 30 percent of GDP?
Burn straw man, burn
The Gobeille decision actually smacks of desperation. The case is the Hail Mary pass that was released two seconds after the clock expired.
The convergence of open data, big data and blockchain technology will lead to the disintermediation of the middlemen in health care faster than the Internet came to life in the mid-1990s. This will turn out to be a white swan that should drive much-needed productivity growth in our national economy. It will appear to have come out of nowhere, but in reality, it will have been borne from the sweat and unrelenting pursuit of progress of free-market policy, a risk-taking private sector and most of all, necessity. The next time you enjoy an Uber ride and reflect on how far superior of an experience it is compared to cabs, ask yourself what health care could look like.
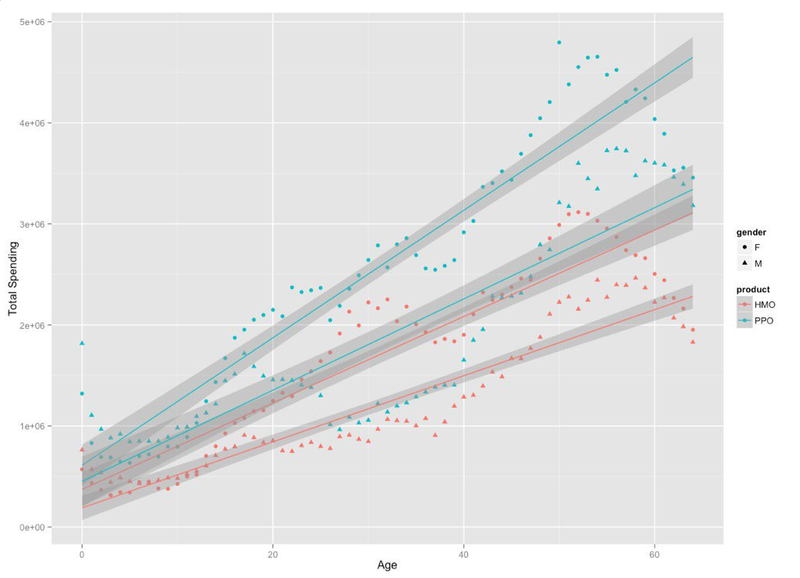
A dataviz created by HealthyHive: HMO and PPO total spending by gender and age; data collected for New Hampshire in 2014. (Image credit: HealthyHive/Twitter)
Live free or die
Our open data company is focusing on the New Hampshire market because its laws provide the easiest access to health care open data. We are just scratching the surface in terms of the types of services that can be provided by refining raw data into actionable intelligence. Our vision of building an integrated financial wellness solution revolves around the immense power contained on a tiny thumb drive (pictured). We calculated that in 1982 purchasing the same amount of storage would have cost around $30 million. Today it is delivered for free. We are building data visualizations to make the raw data more user-friendly with open source software.

The managed care consolidation is leading to fewer players in the New Hampshire marketplace through Anthem and Cigna’s combination. The need for cost transparency has never been greater. While open data startups have been slow to emerge, the potential should not be discounted. Self-funded companies need to understand their employee claims are no longer required to be submitted to the state’s all-payer database. They need to ensure the claims are still submitted by requesting plan administrators submit them anyway. The alternative option of complacency will only continue to stack the decks in favor of obfuscation, confusion and waste on which deep-pocketed insurers thrive.
Interested in writing a guest blog for Sunlight? Email us at guestblog@sunlightfoundation.com

